 PDF(1224 KB)
PDF(1224 KB)


Progressive supranuclear palsy with mimic normal pressure hydrocephalus: A case report and research progress
LIUYing, YANGFu-xia, GUChun-hui, WEIWen-shi
Chinese Journal of Alzheimer's Disease and Related Disorders ›› 2021, Vol. 4 ›› Issue (2) : 134-137.
 PDF(1224 KB)
PDF(1224 KB)
Abbreviation (ISO4): Chinese Journal of Alzheimer's Disease and Related Disorders
Editor in chief: Jun WANG
 PDF(1224 KB)
PDF(1224 KB)
Progressive supranuclear palsy with mimic normal pressure hydrocephalus: A case report and research progress
Objective: To demonstrate a PSP patient which appeared iNPH-like magnetic resonance imaging (MRI) features. Methods: Analyze the diagnosis and treatment of a PSP patient in our hospital, and review the relevant research progress. Results: This patient presented with dyskinesia, stiff limbs, cognitive impairment, dysphagia and dyslalia; The MRI features conclude midbrain atrophy and signal changes.Midbrain atrophy presents “morning glory sign” in axial plane and “hummingbird sign” (HBS)in the median sagittal plane. The third and fourth ventricles were enlarged, the Evan's index>0.34. Cerebrospinal fluid (CSF) tap/shunt treatment in this case resulted in short-term benefits but subsequent deterioration ensued within one year. And the effect of large doses of dopa serazine was not good. Conclusion: This study demonstrated that some PSP patients develop iNPH-like MRI features, suggesting the presence of iNPH-like features in clinical spectrum of PSP. An awareness that PSP can mimic the clinical symptoms of iNPH may help to avoid invasive cerebrospinal fluid shunting procedures.
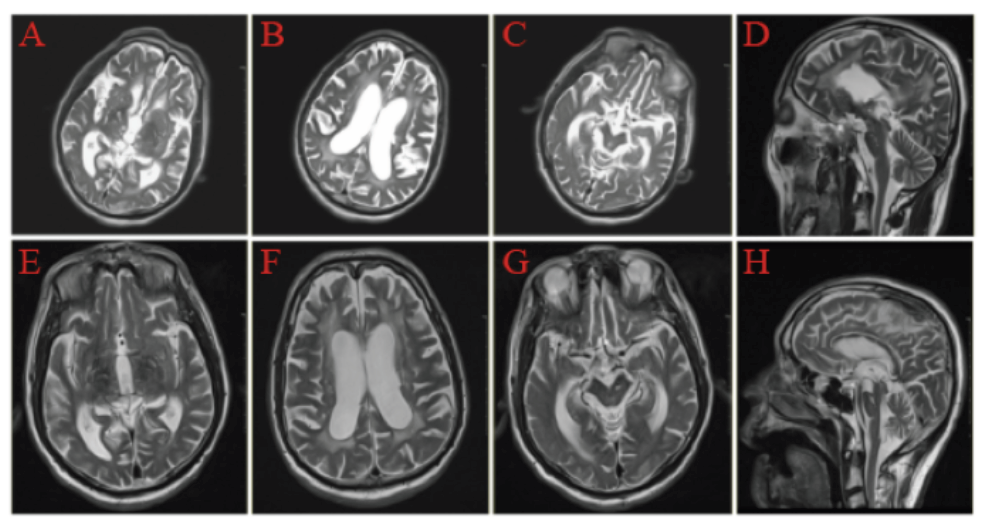
idiopathic normal pressure hydrocephalus / Progressive supranuclear palsy / magnetic resonance imaging
| [1] |
|
| [2] |
|
| [3] |
|
| [4] |
|
| [5] |
|
| [6] |
|
| [7] |
|
| [8] |
Idiopathic normal pressure hydrocephalus (iNPH) is a treatable neurological syndrome in the elderly. Although the magnetic resonance imaging (MRI) findings of tight high-convexity and medial subarachnoid spaces and the ventriculo-peritoneal (VP) shunt with programmable valve are reportedly useful for diagnosis and treatment, respectively, their clinical significance remains to be validated. We conducted a multicenter prospective study (Study of Idiopathic Normal Pressure Hydrocephalus on Neurological Improvement: SINPHONI) to evaluate the utility of the MRI-based diagnosis for determining the 1-year outcome after VP shunt with the Codman-Hakim programmable valve.Twenty-six centers in Japan were involved in this study. Patients aged between 60 and 85 years with one or more of symptoms (gait, cognitive, and urinary problems) and MRI evidence of ventriculomegaly and tight high-convexity and medial subarachnoid spaces received VP shunt using the height/weight-based valve pressure-setting scheme. The primary endpoint was a favorable outcome (improvement of one level or more on the modified Rankin Scale: mRS) at one year after surgery, and the secondary endpoints included improvement of one point or more on the total score of the iNPH grading scale. Shunt responder was defined by more than one level on mRS at any evaluation point in one year.The full analysis set included 100 patients. A favorable outcome was achieved in 69.0% and 80.0% were shunt responders. When measured with the iNPH grading scale, the one-year improvement rate was 77.0%, and response to the surgery at any evaluation point was detected in 89.0%. Serious adverse events were recorded in 15 patients, three of which were events related to surgery or VP shunt. Subdural effusion and orthostatic headache were reported as non-serious shunt-related adverse events, which were well controlled with readjustment of pressure.The MRI-based diagnostic scheme is highly useful. Tight high-convexity and medial subarachnoid spaces, and enlarged Sylvian fissures with ventriculomegaly, defined as disproportionately enlarged subarachnoid-space hydrocephalus (DESH), are worthwhile for the diagnosis of iNPH. This study is registered with ClinicalTrials.gov, number NCT00221091.
|
| [9] |
|
| [10] |
To determine our community's incidence of clinically suspected normal pressure hydrocephalus (NPH), the rate of shunting for NPH, and short- and long-term outcomes of shunting.A retrospective query of the Mayo Clinic medical records linkage system was conducted to identify residents of Olmsted County, Minnesota, undergoing an invasive diagnostic procedure for evaluation of suspected NPH from 1995 through 2003. Among patients with shunts, early- and long-term outcomes were determined via a review of available medical records.Forty-one patients underwent an invasive diagnostic procedure for evaluation of suspected NPH; 13 ultimately received shunts, representing an incidence of 1.19/100,000/year. The incidence of sustained definite improvements at 3 years after shunting was only 0.36/100,000/year. Definite gait improvement was documented in 75% at 3-6 months after shunt placement, although it dropped to 50% at 1 year and to 33% at 3 years. Only 1 of 8 patients with cognitive impairment and 1 of 6 patients with urinary incontinence had definite improvement in these symptoms at 3 years. No patient with moderate to severe postural instability experienced sustained definite improvement in any symptom. Complications occurred in 33% of patients including one perioperative death. Additional or alternative neurologic diagnoses later surfaced in 5 of 12 patients.In this community, NPH is relatively rare with an incidence approximating that of progressive supranuclear palsy in this population. Whereas early gait improvement was common, only one-third of patients enjoyed continued improvement by 3 years; cognition or urinary incontinence was even less responsive long term. Baseline postural instability predicted poor outcome. Clinicians should balance potential benefits of shunting against the known risks.
|
| [11] |
|
| [12] |
Neuropathological features of idiopathic normal-pressure hydrocephalus (iNPH) are poorly characterized. Brain biopsy during life may help in the differential diagnosis of dementia, but post-mortem validation of biopsy findings is scarce. Here we review and report brain biopsy and post-mortem neuropathological findings in patients with presumed NPH.We evaluated 10 patients initially investigated by intraventricular pressure monitoring and a frontal cortical biopsy for histological and immunohistochemical assessment as a diagnostic procedure for presumed NPH.Out of the 10 patients, eight were shunted and seven benefited. Until death, six had developed severe and two mild cognitive impairment. One was cognitively unimpaired, and one was mentally retarded. Three subjects displayed amyloid-β (Aβ) aggregates in their frontal cortical biopsy obtained at the initial procedure. One of these patients developed Alzheimer's disease during a follow-up time of nearly 10 years. One patient with cognitive impairment and NPH suffered from corticobasal degeneration. In six patients various vascular lesions were seen at the final neuropathological investigation. Five of them were cognitively impaired, and in four vascular lesions were seen sufficient in extent to be considered as causative regarding their symptoms.The frequent finding of vascular pathology in NPH is intriguing, suggesting that vascular alterations might be causative of cognitive impairment in a notable number of patients with NPH and dementia. Brain biopsy can be used to detect Aβ aggregates, but neuropathological characteristics of iNPH as a distinct disease still need to be discovered.© 2011 The Authors. Neuropathology and Applied Neurobiology © 2011 British Neuropathological Society.
|
| [13] |
AD pathology is often seen in cortical biopsies of NPH patients. It remains unclear whether these findings are coincidental or causally related. In an aged animal model of NPH, we quantify Abeta and pTau accumulation and describe its temporal and spatial distribution. One-year-old male Sprague-Dawley rats had hydrocephalus induced by cisternal kaolin injection. Immunohistochemistry (IMHC) for AbetaPP, Abeta40, Abeta42 and pTau (epitope pT231) and ELISA for Abeta40, Abeta42 and pT231 were performed on controls and after 2, 6 and 10 weeks of hydrocephalus. Rats had double-label fluorescence IMHC for localization of Abeta42 and pT231. IMHC showed no change in neuronal AbetaPP expression following hydrocephalus. Abeta42 appeared earliest in CSF clearance pathways, p<0.05, and also showed significant rises in perivascular spaces and in cortical parenchyma. Mean ELISA values for Abeta40 and Abeta42 increased three- to four-fold in hydrocephalic rats at 6 and 10 weeks. Abeta40 increased between 2 and 6 weeks (p=0.0001), and remained stable at 10 (p=0.0002); whereas Abeta42 was elevated at 2 weeks (p<0.04) and remained at 6 (p=0.015). PTau at 6 and 10 weeks showed AD-like increased neuronal somatic staining and loss of dendritic staining. ELISA demonstrated increased pT231 in hydrocephalic rats at 10 weeks (p<0.0002). Double-label fluorescence for Abeta42 and pT231 revealed intraneuronal co-localization. Hydrocephalus in the elderly rat, therefore, can induce both Abeta and pTau accumulation. As distinct from brain injury models, no increase in AbetaPP expression was demonstrated. Rather, altered CSF dynamics appears to impair Abeta clearance in this NPH model.2009 Elsevier B.V. All rights reserved.
|
| [14] |
To determine the impact of cortical Alzheimer disease pathology on shunt responsiveness in individuals treated for idiopathic normal pressure hydrocephalus (iNPH), 37 patients clinically diagnosed with iNPH participated in a prospective study in which performance on neurologic, psychometric, and gait measures before and 4 months after shunting was correlated with amyloid β plaques, neuritic plaques, and neurofibrillary tangles observed in cortical biopsies obtained during shunt insertion. No complications resulted from biopsy acquisition. Moderate to severe pathology was associated with worse baseline cognitive performance and diminished postoperative improvement on NPH symptom severity scales, gait measures, and cognitive instruments compared to patients lacking pathology.
|
| [15] |
|
/
| 〈 |
|
〉 |