 PDF(953 KB)
PDF(953 KB)


Clinical and imaging characteristics of 4 patients with primary progressive aphasia
ZHANGMiao, ZHANGHui-hong, CAILi, ZHOUYu-ying
Chinese Journal of Alzheimer's Disease and Related Disorders ›› 2021, Vol. 4 ›› Issue (3) : 201-205.
 PDF(953 KB)
PDF(953 KB)
Abbreviation (ISO4): Chinese Journal of Alzheimer's Disease and Related Disorders
Editor in chief: Jun WANG
 PDF(953 KB)
PDF(953 KB)
Clinical and imaging characteristics of 4 patients with primary progressive aphasia
objective: To analyze the cognitive, linguistic, psychobehavioral symptoms and imaging characteristics of patients with primary progressive aphasia (PPA). Methods: Of 4 patients diagnosed as PPA in the Memory Clinic of Tianjin Huanhu Hospital between April 2014 and March 2018, 1 patient with logopenic progressive aphasia(lvPPA),1 patient with progressive nonfluent aphasia (PNFA), 2 patients with semantic dementia(SD) were identified. Clinical data of the patients were collected. Cognitive function was measured by the Mini-Mental State Examination, Montreal Cognitive Assessment, Clinical Dementia Rating and China Rehabilitation Research Center Aphasia Examination. Also measured by NPI and HAMD depression scale. Brain magnetic resonance imaging was conducted to evaluate the cortex atrophy and medial temporal lobe atrophy. The 18F-fluoro-2-deoxy-D-glucose positron emission tomography (18F-FDG-PET)and Pittsburg Compound B (PiB)PET cerebral imaging were performed in patients with atypical clinical and MRI demonstrations. Results: Among the 4 patients, 3 were male and 1 was female. The onset age was 58~71 years old, and the duration was 1~5 years. All 4 cases were right-handed. All the 4 patients had impaired memory and recall ability, repetitive language disorder and fluency of speech. LvPPA patients is characterized by difficulty in word extraction, naming and retelling, and difficulty in understanding complex sentences. Cognitive impairment progresses rapidly, and the activity of daily living is quickly impaired. Manifests as tension, irritability and fatigue. Head MRI showed bilateral parietal atrophy. PiB-PET shows amyloid deposits. FDG-PET showed decreased metabolism in bilateral temporo-parietal junction, bilateral precuneus and right frontal lobe. The early symptoms of PNFA patients are mainly verbal fluency, speech loss, and language clumsiness. It is difficult to repeat the sentence. The activity of daily living has less impact. The HAMD depression scale showed poor self-awareness. Head MRI showed atrophy of the frontotemporal lobe on the left.FDG-PET showed decreased metabolism in bilateral medial frontal, lateral, bilateral anterior cingulate, bilateral lateral temporal, left medial temporal, bilateral insula and bilateral caudate nucleus, and leftthalamus. The early main symptoms of SD patients are difficulty naming, poor comprehension and difficulty in finding words. The sentence retelling is poor, serious people can not read aloud or transcribe; Picture description and dictation are difficult. The NPI and HAMD scales showed depressive mood, anorexia and sleep disturbance. Head MRI showed bilateral frontal, parietal lobe, left temporal lobe atrophy. FDG-PET showed decreased metabolism of bilateral medial frontal, lateral, bilateral insula, left inner temporal, lateral and left caudate nuclei. Conclusion: PPA patients have different early cognitive,language disorders and mental and behavior disorder due to their anatomical basis. A detailed cognitive,language assessment and neuropsychiatric inventory questionnaire combined with head MRI and FDG-PET can help to identify the diagnosis early.
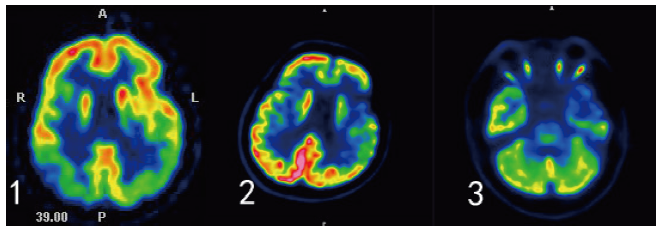
primary progressive aphasia / Dementia / Clinical neuroimage
| [1] |
|
| [2] |
|
| [3] |
|
| [4] |
|
| [5] |
|
| [6] |
|
| [7] |
|
| [8] |
|
| [9] |
Selective disorders in recognition of familiar people have been described in patients with right and left anterior temporal lesions, but the exact nature of these cognitive impairments remains controversial. A clarification of this issue could have theoretical implications, because, according to Snowden et al. [Snowden, J. S., Thompson, J. C., & Neary, D. (2004). Knowledge of famous faces and names in semantic dementia. Brain, 127, 860-872], the pattern of impairment shown by patients with right and left anterior temporal atrophy is inconsistent with unitary, abstract, amodal models of semantic memory. This pattern could, on the contrary suggest a multimodal network, in which the right and left temporal lobes would mainly process and store visual and, respectively, verbal information. I tried to clarify this issue by systematically reviewing: (a) all published individual cases of patients showing a prevalent damage of the anterior parts of the right or left temporal lobes and a selective disorder of famous people recognition; (b) all group studies of patients with right or left temporal lobe epilepsy, which had investigated aspects of famous people recognition impairment. Results of these reviews consistently showed that different patterns of impaired recognition of familiar people can be observed in patients with right and left anterior temporal pathology. These patterns consist of a loss of familiarity feelings and of person specific information retrieval from face stimuli, when the right temporal lobe is damaged and of a prevalent impairment in finding their names when the anterior parts of the left temporal lobe are selectively damaged.
|
| [10] |
The cognitive architecture and neural underpinnings of different semantic domains remains highly controversial. We report two patients with focal temporal lobe atrophy who presented with contrasting and theoretically informative dissociations of person-specific versus general semantic knowledge. Subject J.P. showed severely impaired person-specific semantics, with relative preservation of knowledge about objects and animals, while subject M.A. exhibited the opposite pattern of performance (good knowledge of people in the context of impoverished general semantics). Voxel-based morphometric analysis of MR images in the two cases established predominantly right temporal atrophy associated with J.P.'s deficit for person knowledge and predominantly left temporal atrophy in M.A. who was impaired in general conceptual knowledge.
|
| [11] |
The temporal variant of frontotemporal dementia (tvFTD) features asymmetric anterior temporal/amygdala degeneration as well as ventromedial frontal, insular, and inferoposterior temporal involvement. Left temporal atrophy has been linked to loss of semantic knowledge, whereas behavioral symptoms dominate the right temporal variant.To investigate the first symptoms and the timing of subsequent symptoms in patients with left versus right tvFTD.Twenty-six patients with tvFTD were identified. Six had right > left temporal atrophy (right temporal lobe variant [RTLV]) and were matched with six having comparable left > right temporal atrophy (left temporal lobe variant [LTLV]). Clinical records were reviewed to generate individualized symptom chronologies.In all patients, first symptoms involved semantics (4/6 LTLV, 1/6 RTLV), behavior (4/6 RTLV, 1/6 LTLV), or both (1 LTLV, 1 RTLV). Semantic loss began with anomia, word-finding difficulties, and repetitive speech, whereas the early behavioral syndrome was characterized by emotional distance, irritability, and disruption of physiologic drives (sleep, appetite, libido). After an average of 3 years, patients developed whichever of the two initial syndromes--semantic or behavioral--that they lacked at onset. A third stage, 5 to 7 years from onset, saw the emergence of disinhibition, compulsions, impaired face recognition, altered food preference, and weight gain. Compulsions in LTLV were directed toward visual, nonverbal stimuli, whereas patients with RTLV were drawn to games with words and symbols.The temporal variant of frontotemporal dementia follows a characteristic cognitive and behavioral progression that suggests early spread from one anterior temporal lobe to the other. Later symptoms implicate ventromedial frontal, insular, and inferoposterior temporal regions, but their precise anatomic correlates await confirmation.
|
| [12] |
|
| [13] |
|
/
| 〈 |
|
〉 |