 PDF(1231 KB)
PDF(1231 KB)


Rapidly Progressive Alzheimer's Disease with Extrapyramidal Symptoms: a Case Report
XINGYong-hong, ZHOUYu-ying, FENGKe-ke, CHENGYi-feng, YINShao-ya
Chinese Journal of Alzheimer's Disease and Related Disorders ›› 2021, Vol. 4 ›› Issue (4) : 293-296.
 PDF(1231 KB)
PDF(1231 KB)
Abbreviation (ISO4): Chinese Journal of Alzheimer's Disease and Related Disorders
Editor in chief: Jun WANG
 PDF(1231 KB)
PDF(1231 KB)
Rapidly Progressive Alzheimer's Disease with Extrapyramidal Symptoms: a Case Report
Alzheimer's disease (AD) is a common central nervous system degenerative disease in middle-aged and elderly people, its etiology and pathogenesis are not very clear. Symptoms of Parkinson's disease maybe present in the middle and late stages of Alzheimer's disease, even in the early stages. In this study, we report a case of rapidly progressive Alzheimer's disease with extrapyramidal symptoms, and discuss the problems of diagnosis and treatment.
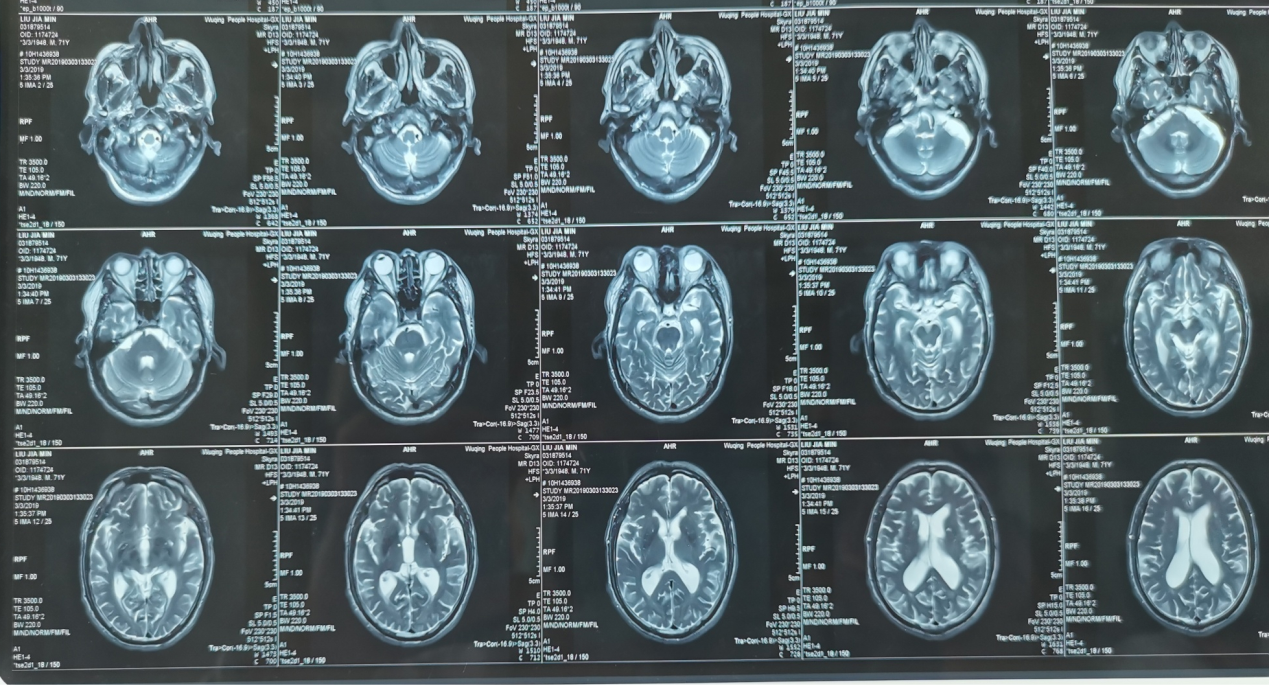
Rapidly progressive Alzheimer's disease / Extrapyramidal symptoms / Deep brain stimulator
| [1] |
Background The number of individuals living with dementia is increasing, negatively affecting families, communities, and health-care systems around the world. A successful response to these challenges requires an accurate understanding of the dementia disease burden. We aimed to present the first detailed analysis of the global prevalence, mortality, and overall burden of dementia as captured by the Global Burden of Diseases, Injuries, and Risk Factors (GBD) Study 2016, and highlight the most important messages for clinicians and neurologists. Methods GBD 2016 obtained data on dementia from vital registration systems, published scientific literature and surveys, and data from health-service encounters on deaths, excess mortality, prevalence, and incidence from 195 countries and territories from 1990 to 2016, through systematic review and additional data-seeking efforts. To correct for differences in cause of death coding across time and locations, we modelled mortality due to dementia using prevalence data and estimates of excess mortality derived from countries that were most likely to code deaths to dementia relative to prevalence. Data were analysed by standardised methods to estimate deaths, prevalence, years of life lost (YLLs), years of life lived with disability (YLDs), and disability-adjusted life-years (DALYs; computed as the sum of YLLs and YLDs), and the fractions of these metrics that were attributable to four risk factors that met GBD criteria for assessment (high body-mass index [BMI], high fasting plasma glucose, smoking, and a diet high in sugarsweetened beverages). Findings In 2016, the global number of individuals who lived with dementia was 43.8 million (95% uncertainty interval [UI] 3 7. 8-51.0), increased from 20.2 million (17. 4-23 5) in 1990. This increase of 117% (95% UI 114-121) contrasted with a minor increase in age-standardised prevalence of 1.7% (1.0-2.4), from 701 cases (95% UI 602-815) per 100 000 population in 1990 to 712 cases (614-828) per 100 000 population in 2016. More women than men had dementia in 2016 (27.0 million, 95% UI 23.3-31. 4, vs 16.8 million, 14.4-19.6), and dementia was the fifth leading cause of death globally, accounting for 2.4 million (95% UI 2.1-2.8) deaths. Overall, 28.8 million (95% UI 24. 5-34. 0) DALYs were attributed to dementia; 6.4 million (95% UI 3.4-10. 5) of these could be attributed to the modifiable GBD risk factors of high BMI, high fasting plasma glucose, smoking, and a high intake of sugar-sweetened beverages. Interpretation The global number of people living with dementia more than doubled from 1990 to 2016, mainly due to increases in population ageing and growth. Although differences in coding for causes of death and the heterogeneity in case-ascertainment methods constitute major challenges to the estimation of the burden of dementia, future analyses should improve on the methods for the correction of these biases. Until breakthroughs are made in prevention or curative treatment, dementia will constitute an increasing challenge to health-care systems worldwide. (C) 2018 The Author(s). Published by Elsevier Ltd.
|
| [2] |
|
| [3] |
|
| [4] |
|
| [5] |
Alzheimer's disease (AD), the most common cause of dementia, typically shows a slow clinical progression over time. 'Rapidly progressive' AD, a variant of the disease characterized by an aggressive course, exhibits distinct clinical, biological, and neuropathological features. Here, we investigate neuropsychological predictors of rapid decline in a group of mild patients with AD.One hundred fifty-three mild patients with AD admitted to a memory disorder clinic and followed for up to 3 years were included in this study. A comprehensive neuropsychological (NP) battery was performed at the time of enrollment. Patients were defined as 'rapidly progressive' if they exhibited a drop of 6 or more points on the Mini Mental State Examination (MMSE) between two consecutive annual visits. This event defined the main outcome in multiple analyses of variance and Cox proportional hazards models that investigated the impact of NP predictors. Categorical principal component analysis (CATPCA) was also employed in order to delineate clusters of NP tests and to test their effect on the outcome.Of 153 subjects, thirty-seven (24%) were classified as 'rapidly progressive'; those subjects showed younger age of symptoms onset compared to slow decliners (68 vs 71.5 years old). Baseline lower performance on a neuropsychological test of naming predicted a rapid decline over the follow-up (P = 0.001). Three clusters of NP were defined by CATPCA: (i) executive/language, (ii) visuospatial memory, and (iii) verbal memory. The executive/language component predicted a rapid decline over the follow-up (P = 0.016).Early executive/language impairment is highly predictive of a rapid progression of AD.© 2015 John Wiley & Sons A/S. Published by John Wiley & Sons Ltd.
|
| [6] |
The analysis of cerebrospinal fluid biomarkers gains importance in clinical routine and is effective in substantiating dementia diagnosis in the differential diagnostic context.We evaluated the levels of β-amyloid (Aβ) 42, Aβ40, tau, and P-tau in a large patient population subdivided into prion diseases, tauopathies, synucleinopathies, and controls. Diagnostic test evaluation was assessed by ROC area under the curve analysis.High tau levels were detected in sporadic Creutzfeldt-Jakob disease (sCJD) and high P-tau levels in Alzheimer's disease (AD) and sCJD. Aβ40 was lower exclusively in prionopathies, but low Aβ42 was detected in AD, sCJD, and Lewy body dementia. When disease groups were stratified according to the underlying proteinopathy, we detected disease-type specificities for all biomarkers. P-tau/tau, Aβ42/40, Aβ42/tau, and Aβ40/tau ratios proved valuable in discriminating disease groups and controls, especially P-tau/tau ratio in the identification of sCJD cases.Combining the biomarker panel allows differentiating between various types of neurodegenerative dementias and contributes to a better understanding of their pathophysiological processes.Copyright © 2015 Alzheimer's Association. Published by Elsevier Inc. All rights reserved.
|
| [7] |
|
| [8] |
|
| [9] |
|
| [10] |
Depression and cognitive disorders, including dementia and mild cognitive impairment, are common disorders in old age. Depression is frequent in dementia, causing distress, reducing the quality of life, exacerbating cognitive and functional impairment and increasing caregiver stress. Even mild levels of depression can significantly add to the functional impairment of dementia patients and the severity of psychopathological and neurological impairments increases with increasing severity of depression. Depressive symptoms may be both a risk factor for, as well as a prodrome of dementia. Major depressive syndrome of Alzheimer's disease may be among the most common mood disorders of older adults. Treating depression is therefore a key clinical priority to improve the quality of life both of people with dementia as well as their carergivers. Nonpharmacological approaches and watchful waiting should be attempted first in patients who present with mild to moderate depression and dementia. In cases of severe depression or depression not able to be managed through nonpharmacological means, antidepressant therapy should be considered.
|
| [11] |
|
| [12] |
Depressive symptoms are very common in chronic conditions. This is true so for neurodegenerative diseases. A number of patients with cognitive decline and dementia due to Alzheimer's disease and related conditions like Parkinson's disease, Lewy body disease, vascular dementia, frontotemporal degeneration amongst other entities, experience depressive symptoms in greater or lesser grade at some point during the course of the illness. Depressive symptoms have a particular significance in neurological disorders, specially in neurodegenerative diseases, because brain, mind, behavior and mood relationship. A number of patients may develop depressive symptoms in early stages of the neurologic disease, occurring without clear presence of cognitive decline with only mild cognitive deterioration. Classically, depression constitutes a reliable diagnostic challenge in this setting. However, actually we can recognize and evaluate depressive, cognitive or motor symptoms of neurodegenerative disease in order to establish their clinical significance and to plan some therapeutic strategies. Depressive symptoms can appear also lately, when the neurodegenerative disease is fully developed. The presence of depression and other neuropsychiatric symptoms have a negative impact on the quality-of-life of patients and caregivers. Besides, patients with depressive symptoms also tend to further decrease function and reduce cognitive abilities and also uses to present more affected clinical status, compared with patients without depression. Depressive symptoms are treatable. Early detection of depressive symptoms is very important in patients with neurodegenerative disorders, in order to initiate the most adequate treatment. We review in this paper the main neurodegenerative diseases, focusing in depressive symptoms of each other entities and current recommendations of management and treatment.
|
/
| 〈 |
|
〉 |