 PDF(1623 KB)
PDF(1623 KB)


A study of social novelty of an Alzheimer's disease model
YEXiao-lian, TAIGuang-ping
Chinese Journal of Alzheimer's Disease and Related Disorders ›› 2021, Vol. 4 ›› Issue (4) : 310-313.
 PDF(1623 KB)
PDF(1623 KB)
Abbreviation (ISO4): Chinese Journal of Alzheimer's Disease and Related Disorders
Editor in chief: Jun WANG
 PDF(1623 KB)
PDF(1623 KB)
A study of social novelty of an Alzheimer's disease model
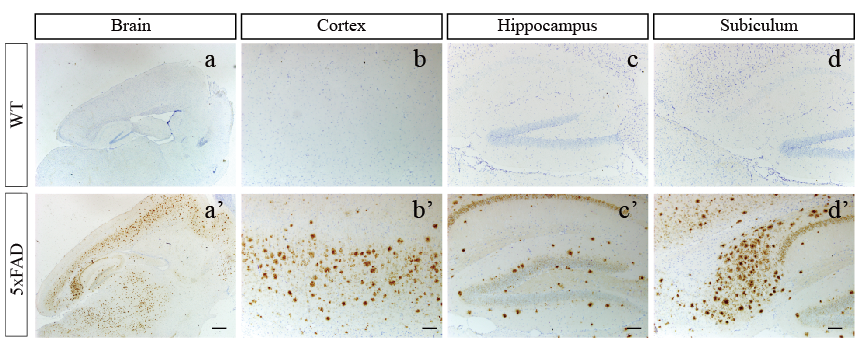
Objective: To explore the social novelty of 5×FAD transgenic mice, and to provide a theoretical basis for the rational application of 5×FAD mouse model to study AD-related behaviors. Methods: Aβ pathology of wild-type mice and 5×FAD mice was examined by immunohistochemical staining; Three chambers tests were carried out to evaluate wild-type and 5×FAD mice aged at 4-5 months. The interaction time between wild-type and 5×FAD mice with S2 mice, the total distance and time in the novelty exploration stage of three chamber tests were recorded. GraphPad Prism 5.0 software, unpaired-t test was performed for statistical analysis. Results: a large number of Aβ plaques were distributed in the cerebral cortex of 5×FAD mice; The average interaction time between wild-type and S1/2 was (95.5 ± 27.22/ 264.6 ± 58.38) s, P < 0.05. The average interaction time between 5×FAD mice and S 1/2 was (91.02 ± 19.49/ 230.2±60.18) s, P < 0.05. There was no difference in interaction time between wild-type and 5×FAD mice with S2, P > 0.05. The total distance of wild-type mice and 5×FAD mice during the tests was (10710 ± 1781/ 9017 ± 1402) mm respectively, P > 0.05. The average speed of wild-type and 5×FAD mice in the equipment was (47.7 ± 5.453/ 37.24 ± 4.590) mm/s respectively, P > 0.05. Conclusion: 5×FAD mice displayed severe Aβ plaques pathology at the age of 5 months, and their social novelty behavior is no different from that of wild-type mice.
Alzheimer's disease / transgenic mice / Aβ plaque / social novelty
| [1] |
Alzheimer's Association. 2015 Alzheimer's disease facts and figures[J]. Alzheimer's & dementia : the journal of the Alzheimer's Association, 2015, 11(3): 332-384.
|
| [2] |
|
| [3] |
The prevalence of Alzheimer's disease is similar across ethnic groups. To our knowledge, no comparison of behavioral symptoms has been addressed.This cross-sectional, retrospective, descriptive study compares neuropsychiatric symptoms of Chinese subjects with Alzheimer's disease (AD) at tertiary care centers in Taiwan and Hong Kong against Caucasian subjects in Los Angeles, California. We compared the frequency and severity of symptoms and caregiver responses to neuropsychiatric symptoms of AD using the Neuropsychiatric Inventory (NPI). We hypothesized that Chinese patients do not seek care unless they have high severity of neuropsychiatric symptoms and that Caucasian Americans do not wait for behavioral disturbances to develop before coming to medical attention.The Caucasian sample had the highest mean educational level and mildest Clinical Dementia Rating (CDR) scale distributions of all four groups. Older age and lower educational levels contributed to higher CDR scale scores, which in turn correlated with higher total NPI scores. Only one of the Chinese samples had a higher frequency of severe neuropsychiatric symptoms than the Caucasian sample. Chinese caregivers reported anxiety and delusions more frequently (58.1%) than Caucasians (37.3% and 39.6%; chi(2), p < 0.01 and p < 0.05, respectively). Caucasians reported appetite changes (47.3%) and apathy (59.2%) more frequently than the Chinese samples (chi(2), p < 0.05 and p < 0.01, respectively). Caregivers at all four centers were distressed by behaviors qualified as severe.We found support for our hypothesis, in that Chinese subjects presented during a more severe stage of dementia than American subjects, but the delay in seeking care could not be correlated with significant differences in neuropsychiatric profiles of the demented subjects. Other barriers to dementia care warrant investigation.Copyright 2002 John Wiley & Sons, Ltd.
|
| [4] |
Neuropsychiatric symptoms are common in Alzheimer's disease. Personality changes, mood disturbance, and psychosis are frequently seen and may coexist in the same patient. Neuropsychiatric symptoms may signal the onset of disease and often fluctuate and recur. These symptoms are associated with a more rapid cognitive and functional decline that can lead to institutionalization. Cholinergic therapy, disease-modifying therapy, and psychotropic medications can improve these symptoms.
|
| [5] |
The Neuropsychiatric Inventory (NPI) was developed to assess psychopathology in dementia patients. It evaluates 12 neuropsychiatric disturbances common in dementia: delusions, hallucinations, agitation, dysphoria, anxiety, apathy, irritability, euphoria, disinhibition, aberrant motor behavior, night-time behavior disturbances, and appetite and eating abnormalities. The severity and frequency of each neuropsychiatric symptom are rated on the basis of scripted questions administered to the patient's caregiver. The NPI also assesses the amount of caregiver distress engendered by each of the neuropsychiatric disorders. A total NPI score and a total caregiver distress score are calculated, in addition to the scores for the individual symptom domains. Content validity, concurrent validity, inter-rater reliability, and test-retest reliability of the NPI are established. Different neurologic disorders have characteristic neuropsychiatric manifestations and distinctive NPI profiles. The NPI is sensitive to treatment effects and has demonstrated the amelioration of behavioral symptoms in Alzheimer's disease by cholinergic agents. The NPI is a useful instrument for characterizing the psychopathology of dementia syndromes, investigating the neurobiology of brain disorders with neuropsychiatric manifestations, distinguishing among different dementia syndromes, and assessing the efficacy of treatment.
|
| [6] |
We developed a new instrument, the Neuropsychiatric Inventory (NPI), to assess 10 behavioral disturbances occurring in dementia patients: delusions, hallucinations, dysphoria, anxiety, agitation/aggression, euphoria, disinhibition, irritability/lability, apathy, and aberrant motor activity. The NPI uses a screening strategy to minimize administration time, examining and scoring only those behavioral domains with positive responses to screening questions. Both the frequency and the severity of each behavior are determined. Information for the NPI is obtained from a caregiver familiar with the patient's behavior. Studies reported here demonstrate the content and concurrent validity as well as between-rater, test-retest, and internal consistency reliability; the instrument is both valid and reliable. The NPI has the advantages of evaluating a wider range of psychopathology than existing instruments, soliciting information that may distinguish among different etiologies of dementia, differentiating between severity and frequency of behavioral changes, and minimizing administration time.
|
| [7] |
|
| [8] |
|
| [9] |
|
| [10] |
|
| [11] |
|
| [12] |
|
| [13] |
|
| [14] |
|
| [15] |
In a previous publication [Deacon RMJ, Cholerton LL, Talbot K, Nair-Roberts RG, Sanderson DJ, Romberg C, et al. Age-dependent and -independent behavioral deficits in Tg2576 mice. Behav Brain Res 2008;189:126-38] we found that very few cognitive tests were suitable for demonstrating deficits in Tg2576 mice, an amyloid over-expression model of Alzheimer's disease, even at 23 months of age. However, in a retrospective analysis of a separate project on these mice, tests of social memory and open field habituation revealed large cognitive impairments. Controls showed good open field habituation, but Tg2576 mice were hyperactive and failed to habituate. In the test of social memory for a juvenile mouse, controls showed considerably less social investigation on the second meeting, indicating memory of the juvenile, whereas Tg2576 mice did not show this decrement.As a control for olfactory sensitivity, on which social memory relies, the ability to find a food pellet hidden under wood chip bedding was assessed. Tg2576 mice found the pellet as quickly as controls. As this test requires digging ability, this was independently assessed in tests of burrowing and directly observed digging. In line with previous results and the hippocampal dysfunction characteristic of aged Tg2576 mice, they both burrowed and dug less than controls.
|
| [16] |
|
| [17] |
|
| [18] |
|
| [19] |
|
/
| 〈 |
|
〉 |